Until dementia do them part Bright retirement plans slowly, inexorably, frighteningly fade to black for once-active middle-age couple
Read this article for free:
or
Already have an account? Log in here »
To continue reading, please subscribe:
Monthly Digital Subscription
$1 per week for 24 weeks*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Billed as $4.00 plus GST every four weeks. After 24 weeks, price increases to the regular rate of $19.95 plus GST every four weeks. Offer available to new and qualified returning subscribers only. Cancel any time.
Monthly Digital Subscription
$4.99/week*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Billed as $19.95 plus GST every four weeks. Cancel any time.
To continue reading, please subscribe:
Add Free Press access to your Brandon Sun subscription for only an additional
$1 for the first 4 weeks*
*Your next subscription payment will increase by $1.00 and you will be charged $16.99 plus GST for four weeks. After four weeks, your payment will increase to $23.99 plus GST every four weeks.
Read unlimited articles for free today:
or
Already have an account? Log in here »
Hey there, time traveller!
This article was published 17/03/2018 (2956 days ago), so information in it may no longer be current.
At the peak of his career, Doug McLean was overseeing a staff of 25 at IBM in Winnipeg and winning awards for his work.
“I was having a blast,” he says at the kitchen table of an east Winnipeg condo he shares with his wife Sandy and rescue dog Ruby.
Then, in his early 50s, he struggled at work.

“Schedules were really screwed up. Simple executive functions are gone. There was a lot of frustration,” he says, leaning into the conversation. “I loved my job but I had to quit. When you can’t do two-plus-two or five-plus-five, you’re done.
“It sucks. The worst part is, you don’t know what’s going on. What used to be normal isn’t normal anymore.”
It took several agonizing years of misdiagnoses before he found out what was wrong.
Doug, who is just 61, has Lewy body dementia. It causes a progressive decline in mental abilities. It affects the areas of the brain that involve thinking and movement. The dementia occurs because of abnormal protein deposits — called Lewy bodies, after Friederich Lewy, the scientist who first described them — inside the brain’s nerve cells that interrupt the brain’s messages.
“I am going to die of the disease,” Doug says without a trace of self-pity.
● ● ●
Over the next two decades, Manitoba will be hit by a dementia tsunami.
By 2038, the number of aging baby boomers with some form of dementia is expected to double, to more than 40,000.
Medical experts and people struggling with the disease say not enough is being done to prepare an already-strained health-care system for what’s coming.
“There are more people at risk every year we get more into the baby boom,” says Dr. Barry Campbell, a geriatric psychiatrist and well-known Manitoba dementia expert.
“More than ever, there’s a concern that we’ve got to do things better so we don’t get overwhelmed.”
Some Manitobans are already feeling overwhelmed.
● ● ●
“There’s no happy story here,” Doug says. It’s what his wife Sandy describes as an increasingly rare “good day”; his mood is upbeat and his train of thought stays on the rails.
He’s waiting for his ride to take him on an afternoon outing.
“Now, a lot of it is finding ways to have positive outcomes in your day-to-day life. It’s important to do that.”
But it’s far from easy.
“The hardest thing is, I look normal and I could be in a situation where I look around and say, ‘Oh, Christ, where am I?’ That’s the scary part,” he says.
That’s why he enjoys going to Actionmarguerite, a facility in St. Boniface that offers a day program for adults with cognitive difficulties. Doug feels a sense of relief and belonging when he joins the group. He can play shuffleboard and socialize without anyone judging him.

It’s one of four outings a week for Doug, who gets picked up at home by paid companion Howard Andersen.
“He’s my lifeline,” says Sandy. The McLeans are allotted 20 hours of help each week through provincial “self and family-managed home care.” That’s where Andersen comes in; they hired him through a private agency to spend that time taking Doug out for activities, giving Sandy some respite.
“With home care, they come and sit in your house,” she says. “That wouldn’t be good for Doug. He’s active — he likes to get out and do things.”
Andersen also takes Doug to an Alzheimer Society of Manitoba support group downtown, swimming and to visit Doug’s mom, who is in her 90s. Sometimes, the McLeans will buy tickets for Doug and Andersen to attend a Moose game together.
“Doug and Howard clicked,” she says. “He’s around the same age as Doug and they get along great.”
● ● ●
Sandy and Doug used to do everything together. They met online in 2005 after both came out of long marriages, 25 years each. Sandy says she was immediately attracted to Doug.
“It was an instant thing. He was, and still is, very good looking. He was very nice, very easygoing,” she says. “Doug was a very confident person. He was a manager at IBM. I was a supervisor at the tax centre.”
Both were workaholics. Both have grown children living in Winnipeg.

“We wanted the same thing in our retirement — to live outside the city and snowbird in the winter. Everything lined up,” she says.
They bought property in Pinawa, spending every weekend there preparing to make it their summer home. They had season tickets for the Royal Manitoba Theatre Centre. They travelled a lot. Trim, fit and tanned, they were sun-worshippers who enjoyed basking by the pool during winter vacations to Mexico.
Then, the sun began to set on their bright future.
“Just after we got married in the summer of 2008, I noticed a lot of personality changes,” Sandy says. “He went from a super-confident, almost arrogant person — especially at work, where he won all these awards — to someone who got a new project at work and was super-stressed. It was the first time I saw him stressed about anything. I didn’t worry until 2009, when he was packaged out (his employer gave him severance and showed him the door).
“It was horrible,” Sandy continues. “Work was his life.”
Doug applied for other jobs and was often hired. He would try them out, then quit. That went on for nearly two years. It was like he was having a nervous breakdown, Sandy says.
“At 50-something, I didn’t know you could get dementia,” she says.
It wasn’t Doug’s memory, but his executive functioning — his mental flexibility — that faded, leaving him struggling.
In 2009, they got a referral to see a neurologist. It didn’t go well. The specialist seemed to think Doug wasn’t trying, Sandy says. He was sent for a neuro-psych test and and that didn’t go well, either, she says.
“During the process I went through trying to find out what was going wrong, I blew up,” Doug says, adding he couldn’t perform the tests he was asked to do.
Rather than letting Doug take a break and calm down, they showed him the door, Sandy says.
“They stopped the testing and wouldn’t let him redo it…. They told us to get his stress under control.”
The specialist treated him like he had a bad attitude and anxiety, not someone with a cognitive impairment, Doug says.

“He diminished what was happening to me. I know there’s something wrong with me. I know in my head that this is not normal.”
Sandy felt frustrated and helpless. “We kind of floundered for another year or two.”
Doug got a minimum-wage guard job but struggled to understand the work schedule. He was angry, bitter and doing less. He was also becoming more confused. When they decided to paint their ceiling, he taped the ceiling rather than the walls. When they rented a U-haul, he went to put gas in it and came back furious, saying it didn’t have a gas gauge.
“He would come home with crazy stories,” she says. “He would phone me 10 times a day at work and then forget to pick me up from work.”
In a search for answers, Doug went to the Anxiety Disorders Clinic. At his first visit, the doctor said it wasn’t anxiety, but rather early onset Alzheimer’s.
Doug was referred to Campbell, a geriatric psychiatrist. By this time, Doug couldn’t tell time on an analog clock. But they had to go back to the original neurologist for a diagnosis.
The neurologist said Doug didn’t present as someone with Alzheimer’s. “He decided again that he felt Doug was stressed out or had another mental disorder,” Sandy says.

Doug was sent for another neuro-psych test and this time, a woman administered the test, stopping when he got flustered and needed a break. That was followed by a PET (positron emission tomography) scan.
“It showed damage all over his brain,” Sandy says. In 2014, six years after his cognitive problems started to show, Doug was diagnosed with Lewy body dementia.
“He thought he was going insane and feeling suicidal,” she says. “A lot of that was stemming from not knowing what was wrong with him, from people not telling him.”
Once he got the diagnosis, he was able to take medication that helped significantly. But those drugs are becoming less effective as the disease progresses, she says.
“Every day’s a different day. In the first few years, when Doug got on the right pills we did some things on our bucket list. We went to Scotland and on an Alaskan cruise.” she says. “We’ve done some really nice things.”
● ● ●
Getting a diagnosis of LBD brought some relief, but knowing there is no cure and the disease will only get worse was devastating, says Sandy, who was diagnosed with a heart problem and had to leave her own job in 2015.
Doug, meanwhile, was frustrated and angry.
“I spent a lot of time tip-toeing around,” she said. “He’s got a bad temper — you do everything to not rock the boat.”
In December 2016, she had to call 911 when his anger erupted and he hurt her.
At times, he’s turns his rage on himself. He’s been suicidal, Sandy says, who stopped him from jumping ship on the Alaskan cruise.
They can’t travel anymore.

He can’t make coffee, but can still talk. However, the man with a vocabulary that once wowed his wife now has to pause mid-sentence to find the right word.
“His confidence is not there,” she says.
Doug has a cellphone that he can’t use, but carries as a tracking device. The couple got an eight-year-old rescue dog, Ruby, a few months ago. “She’s been a godsend,” Sandy says.
Doug sometimes can’t see the playful, affectionate pooch on the floor because Lewy body dementia affects his vision and depth perception. Sandy puts bright green masking tape on fridge and cupboard shelves and the basement stairs so that Doug can see them.
“With Lewy body, he could have motor issues, stiffening and tremors one day — be a zombie and shuffle around — and then 24 hours later, he could be running.”
Another troubling LBD symptom is a sleep disorder during which people physically act out their dreams. One night Doug dreamed he was being chased by a bear and got out of bed and was running around the house. Another time, Sandy was awakened by Doug with his hands around her throat.
“He physically attacked me a couple of times during the night,” she says. “You could see that he had to be sleeping.” He’s now on medication, which has helped. And they now sleep in separate rooms.

Sandy has reached out for help but it’s been a tough stretch — from getting the initial diagnosis to managing day to day as his primary caregiver.
At first, they went together to a weekly Alzheimer Society of Manitoba support group, which was beneficial. The non-profit organization points people in the right direction for help, but can’t navigate the system with each individual, says Sandy, who struggled to figure that out for herself.
She stopped going to the support group after two years because she felt she was giving more support than she was receiving and she feels she no longer has any to spare. Doug goes on his own with his companion.
They face their next step with trepidation. She doesn’t want Doug to move into a personal-care home, but looking after him on her own is exhausting.
“One of the hardest parts of being a caregiver to someone with dementia is that you need to be hyper-vigilant at all times,” she wrote in an email after being interviewed. The person with the disease doesn’t recognize danger anymore and can injure themselves at any time, she said.
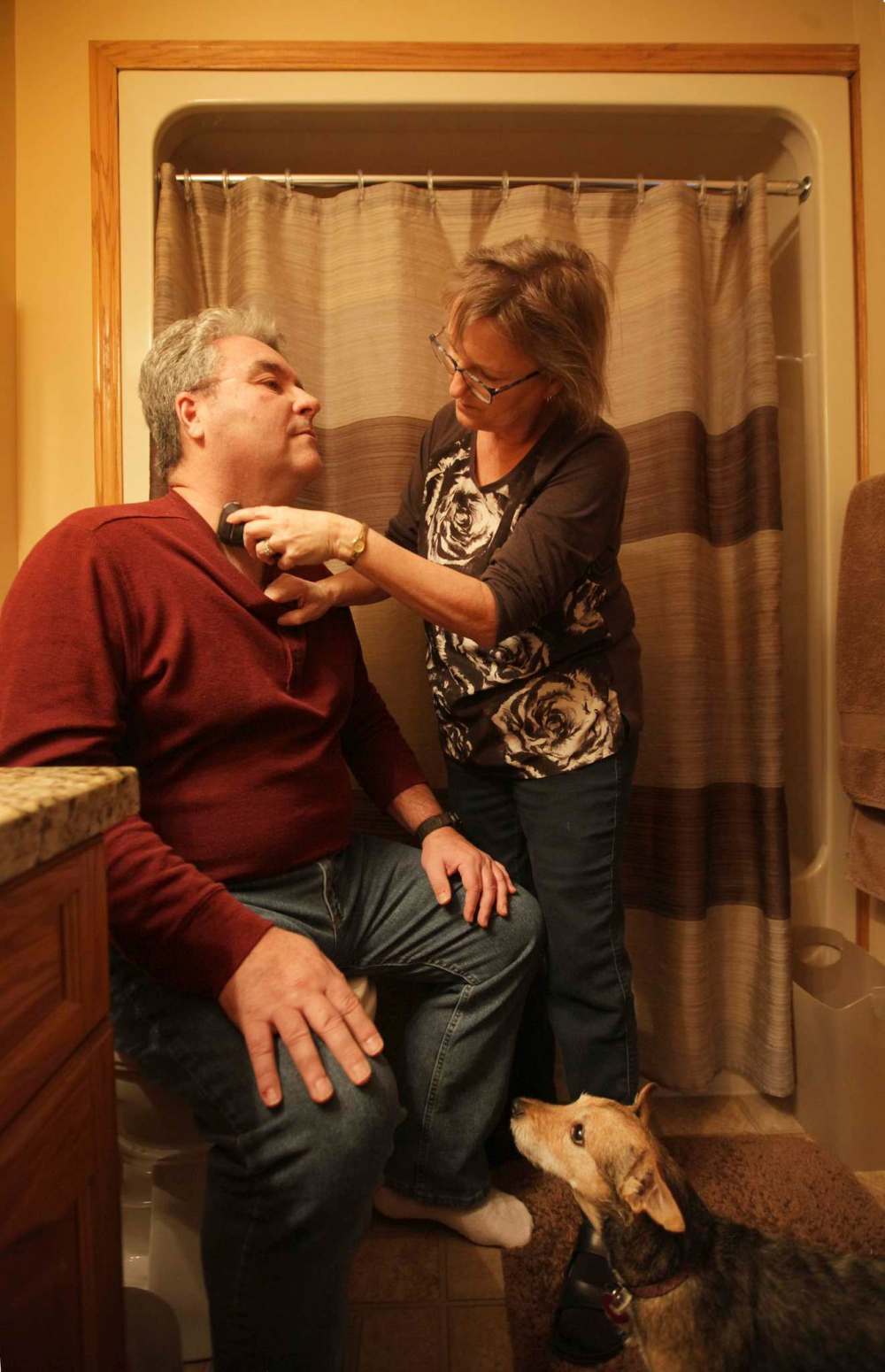
“I caught him using his moustache groomer as a toothbrush. He broke the groomer but luckily did not break his teeth.”

Sandy says she was putting off shoulder surgery because she will be in a sling for a few weeks and worries about how she’ll manage caring for herself and Doug.
Doug understands that his situation will never improve. He wishes he could be euthanized when he’s in the final stages of his disease, as federal law now allows people with other terminal and debilitating illnesses to apply for assisted death.
But that’s not the case for those who have been diagnosed with dementia. Doug says people in his situation should be allowed to arrange for it while they still have the intellectual capacity to understand what they’re doing.
“I know my life is going to be the shits. I know I’m going to get worse. If I’m in a situation where I’m not aware and not cognitive of my situation, I don’t want to be here.
“Our system is buggered up.”




Carol Sanders
Legislature reporter
Carol Sanders is a reporter at the Free Press legislature bureau. The former general assignment reporter and copy editor joined the paper in 1997. Read more about Carol.
Every piece of reporting Carol produces is reviewed by an editing team before it is posted online or published in print — part of the Free Press‘s tradition, since 1872, of producing reliable independent journalism. Read more about Free Press’s history and mandate, and learn how our newsroom operates.
Our newsroom depends on a growing audience of readers to power our journalism. If you are not a paid reader, please consider becoming a subscriber.
Our newsroom depends on its audience of readers to power our journalism. Thank you for your support.


