Another day, another COVID record 146 new cases highlight virus’s spread in Winnipeg over last six weeks
Read this article for free:
or
Already have an account? Log in here »
To continue reading, please subscribe:
Monthly Digital Subscription
$1 per week for 24 weeks*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Billed as $4.00 plus GST every four weeks. After 24 weeks, price increases to the regular rate of $19.95 plus GST every four weeks. Offer available to new and qualified returning subscribers only. Cancel any time.
Monthly Digital Subscription
$4.99/week*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Billed as $19.95 plus GST every four weeks. Cancel any time.
To continue reading, please subscribe:
Add Free Press access to your Brandon Sun subscription for only an additional
$1 for the first 4 weeks*
*Your next subscription payment will increase by $1.00 and you will be charged $16.99 plus GST for four weeks. After four weeks, your payment will increase to $23.99 plus GST every four weeks.
Read unlimited articles for free today:
or
Already have an account? Log in here »
Hey there, time traveller!
This article was published 14/10/2020 (2017 days ago), so information in it may no longer be current.
In early September, cases of the novel coronavirus were scattered across Manitoba, reaching 20 or 30 a day. Sixteen people had died from the virus since the first case was identified in March, and hospitalizations in the province remained low.
Fast forward six weeks. COVID-19 cases have spiked in Winnipeg, with more cases recorded in the last six weeks than in the previous six months. Twenty-three people have died since the beginning of September, accounting for nearly two-thirds of the province’s COVID-19 deaths.
And on Wednesday, the province announced 146 new cases of the virus — the highest daily total recorded in Manitoba.
But those familiar with the deadly contagion say the mounting COVID-19 wave Winnipeg is riding isn’t unexpected.
“Given that our immune system is naive, given that many people have been shut away from each other from a long period of time, it’s not surprising from an epidemiological perspective that when you allow more people to get back together without immunity, that you would see more cases,” said epidemiologist Cynthia Carr.
“It’s just right now we have to figure out how to get on top of this in Winnipeg without going to a red zone.”
On Wednesday, Manitoba announced a five-day test positivity rate of 4.4 per cent, the highest it’s been since the province began reporting that figure.
Twenty-seven people were in hospital with COVID-19 Wednesday, including three in intensive care. Two deaths, a man in his 80s and woman in her 70s, both from Winnipeg, were also announced. Both were residents of Parkview Place Long Term Care Home.
The new cases were reported in the following regions: Winnipeg (114), Prairie Mountain (two), Southern Health-Sante Sud (17), Interlake-Eastern (nine), and northern (four). Of the new cases, 39 were identified Monday and 107 were identified Tuesday.
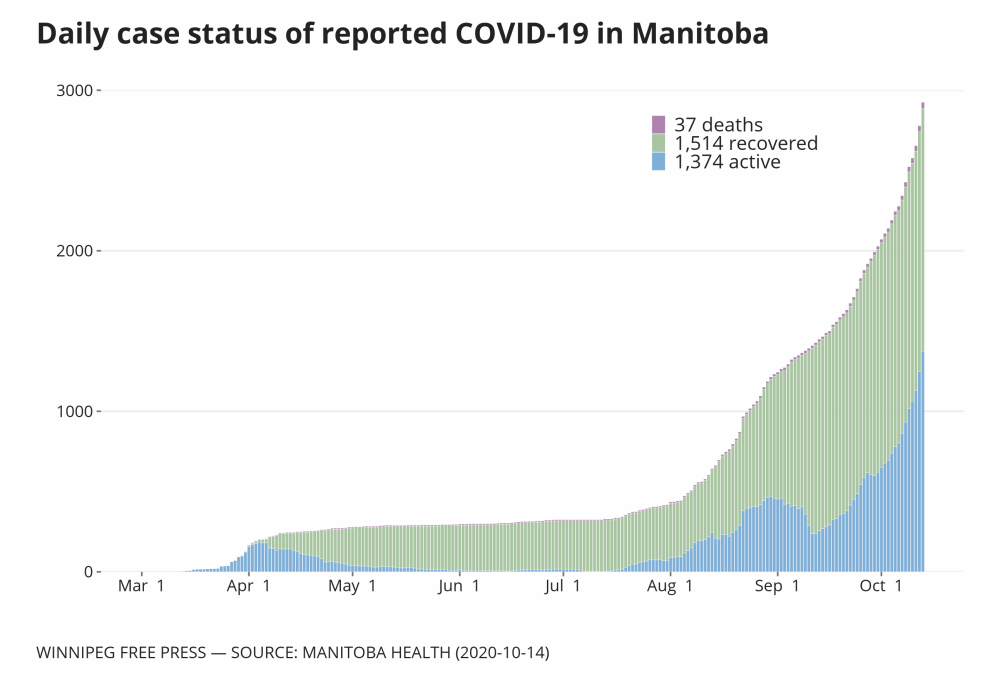
A total of 1,374 active cases were reported by the province Wednesday, though public health officials admit there is a lag in reporting recoveries, of which there were 1,514.
While the new cases reported Wednesday marked a high point, Carr cautioned against using daily numbers as a pandemic barometer.
Rather, the weekly increase in cases — which in Manitoba have doubled every two weeks since Sept. 6 — provides a better picture of how the virus is spreading in the community.
In the week of Sept. 6, 108 new cases were reported in Manitoba. Two weeks later, on Sept. 20, 294 new cases were added to the tally. By Oct. 4, another 502 cases were reported.
“We’re definitely seeing quite an increase ongoing, even since Sept. 28, when we went into code orange,” Carr said. “Our average new (daily) cases per 100,000 residents was 4.5 and now it’s more than doubled to 10.1.”
With the changes in weather, people getting together in groups, using public transit more frequently and heading to gyms, gatherings, schools and workplaces, more people are potentially exposing themselves to the virus in the community, Carr said.
Carr said the reproduction rate of the virus is 2.3 on average, meaning a person infected is expected to spread it to at least two others, when precautions or restrictions are not in place.
“We saw very low numbers over the summer which were great, but now with the fall, with more opportunity for spread, we’re seeing in our… numbers go up again, but it doesn’t mean that’s destiny because it’s not happening in every area,” she said.
Dr. Joel Kettner, an associate professor in the department of community health sciences at the University of Manitoba, said the surge in cases is to be expected, in some respects.
It is difficult, however, to know the extent to which the province’s strategies to reopen schools and the economy have had in containing COVID-19.
“If we think we can predict how this is going to go, I think we’re not really appreciating the complexity of the spread of a virus in a social animal like humans,” Kettner, the province’s former top doctor, said.
As for the summer lull in cases in Manitoba, it could be attributed to the number of tests performed, behaviour, restrictions or other biological factors, Kettner said.
“We hope that distancing, masks, handwashing and not going to work while you’re sick and all of that, slows down or interrupts some of that transmission,” Kettner said. “I don’t want to discount or ignore that there was probably a change of behaviour in the period that has the lowest rate of cases.”
danielle.dasilva@freepress.mb.ca
History
Updated on Thursday, October 15, 2020 6:41 PM CDT: Minor editing