Third wave of pandemic flows into familiar territory
Read this article for free:
or
Already have an account? Log in here »
To continue reading, please subscribe:
Digital Subscription
One year of digital access for only $75*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Billed as $5.77 plus GST every four weeks. After 52 weeks, price increases to the regular rate of $19.95 plus GST every four weeks. Offer available to new and qualified returning subscribers only. Cancel any time.
Monthly Digital Subscription
$4.99/week*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Billed as $19.95 plus GST every four weeks. Cancel any time.
To continue reading, please subscribe:
Add Free Press access to your Brandon Sun subscription for only an additional
$1 for the first 4 weeks*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Your next Brandon Sun subscription payment will increase by $1.00 and you will be charged $17.95 plus GST for four weeks. After four weeks, your payment will increase to $24.95 plus GST every four weeks.
Read unlimited articles for free today:
or
Already have an account? Log in here »
Hey there, time traveller!
This article was published 21/04/2021 (1856 days ago), so information in it may no longer be current.
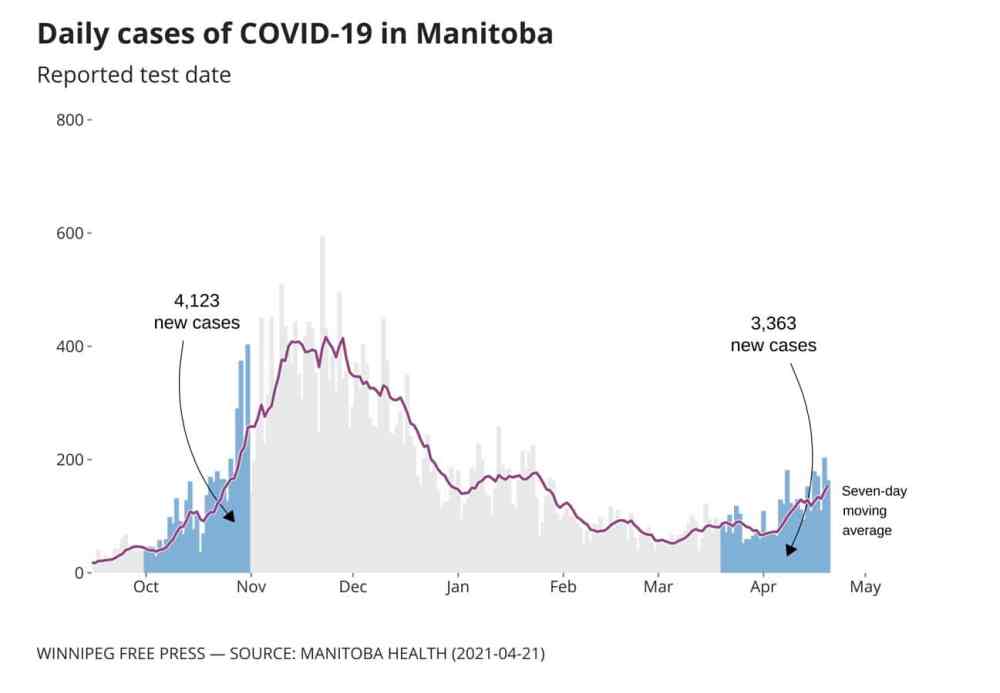
On Tuesday, Manitoba recorded its highest daily new COVID-19 case count in nearly three months: 211.
In as little as 10 days, that number could double — and 400 cases each day could overwhelm the health-care system, based on what happened in fall 2020, says Dr. Anand Kumar, attending ICU physician at the Health Sciences Centre in Winnipeg.
“We’re on the cusp of a major wave again, and I think that short of extremely tight restrictions, it’s going to be difficult to stop it,” Kumar says.

He and some of his colleagues have been urging the Manitoba government to implement tighter restrictions since the second wave hit in the fall. He’s criticized pandemic responses that don’t adopt a “COVID Zero” philosophy as a way to focus on locking down to keep case counts low and easily contact-traceable.
But a “COVID Zero” approach, similar to the bubble strategy adopted in the Atlantic provinces and countries such as New Zealand and Australia, wouldn’t work in Manitoba now, says deputy chief provincial public health officer Dr. Jazz Atwal.
It would mean a complete lockdown until cases get as close to zero as possible.
“That is an extreme strategy. It just won’t be a viable option, to be quite frank, from a public health perspective. We have transmission in the community. We have borders that are open, we rely on a lot of movement of individuals that are critical to our livelihoods from a goods and services perspective that move across the country. We aren’t an island,” Atwal says.
“Outside of that, it’s really hard to go back to that at this point. Very extreme measures would have to occur, but they would have to occur at every jurisdiction; federal (and) provincial level.”
Here’s a look at how the beginning of Manitoba’s third wave compares to the start of its second:
Vaccines, variants race against time
Younger Manitobans are getting sicker with highly-contagious COVID-19 variants and are more likely to be admitted to hospital than they were during the first and second waves of the pandemic.
Vaccines aren’t getting out fast enough to get ahead of the spread of these more infectious variants. B.1.1.7 is becoming the dominant strain in Manitoba and already accounts for the majority of new cases in Winnipeg.
However, research has shown existing vaccines are effective against B.1.1.7, and this week, vaccine eligibility was expanded significantly.
Manitobans 40 and up with no underlying health conditions are booking appointments to receive the AstraZeneca vaccine through local pharmacies. On Wednesday, the province opened vaccine appointments at its immunization clinics for all Manitobans 50 and older, and First Nations people 30-plus.
Front-line police and firefighters are also now eligible to make appointments, and the province plans to open vaccine clinics in “high-risk” areas.
On Tuesday, the province announced a plan to vaccinate truck drivers making essential trips across the U.S. border.
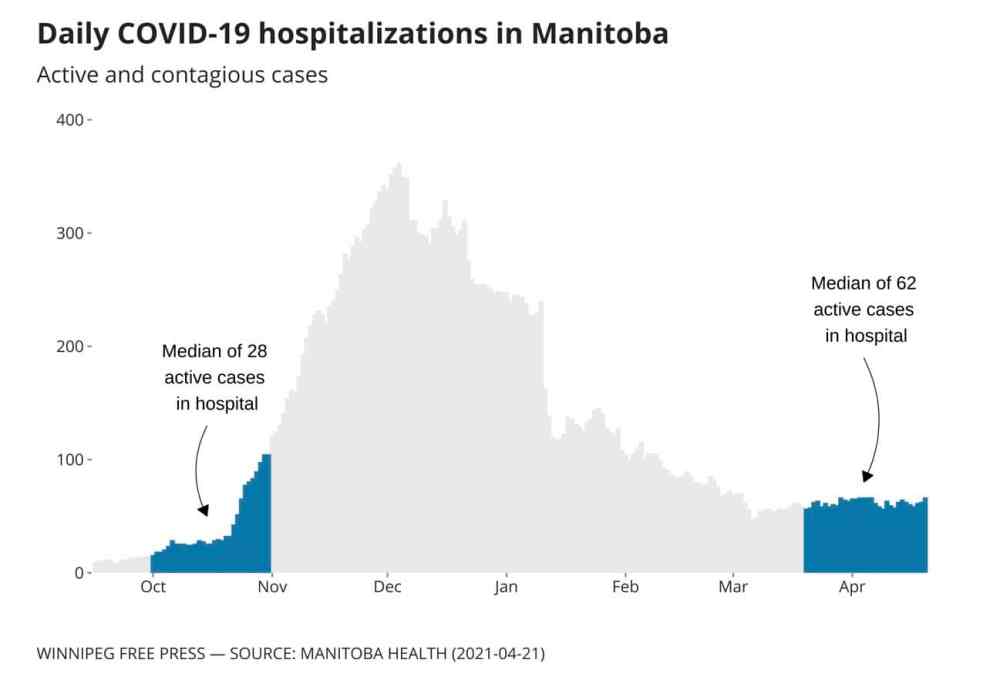
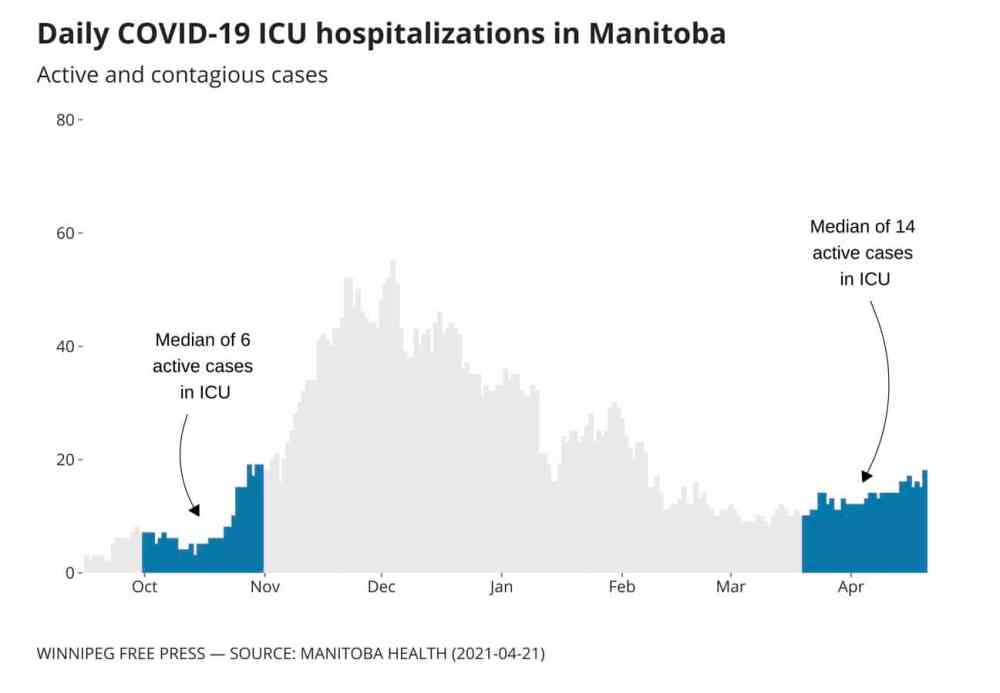
Hospitalizations rising, staff burned out
Hospitalization rates stabilized earlier this year, but didn’t drop back to pre-second-wave levels before the third wave began. This time around, as the elderly population is largely vaccinated and younger people are entering the ICU, burnout is increasing.
“We’ve learned over and over not to underestimate this virus, and we’re also dealing with a bit of a new beast with all these variants that are coming around. Perhaps even most importantly, we’re dealing with an exhausted health-care workforce,” St. Boniface Hospital microbiologist Dr. Philippe Lagacé-Wiens says.
Nurses are rapidly retiring or moving out of critical care and trying to find work in private practice or less stressful areas, according to Manitoba Nurses Union president Darlene Jackson.
“It’s extremely worrying hearing from nurses that they are exhausted and don’t know how much longer they can keep up with this pace, especially going into a third wave, seeing the variant that’s out there and the climb in our numbers,” she says.
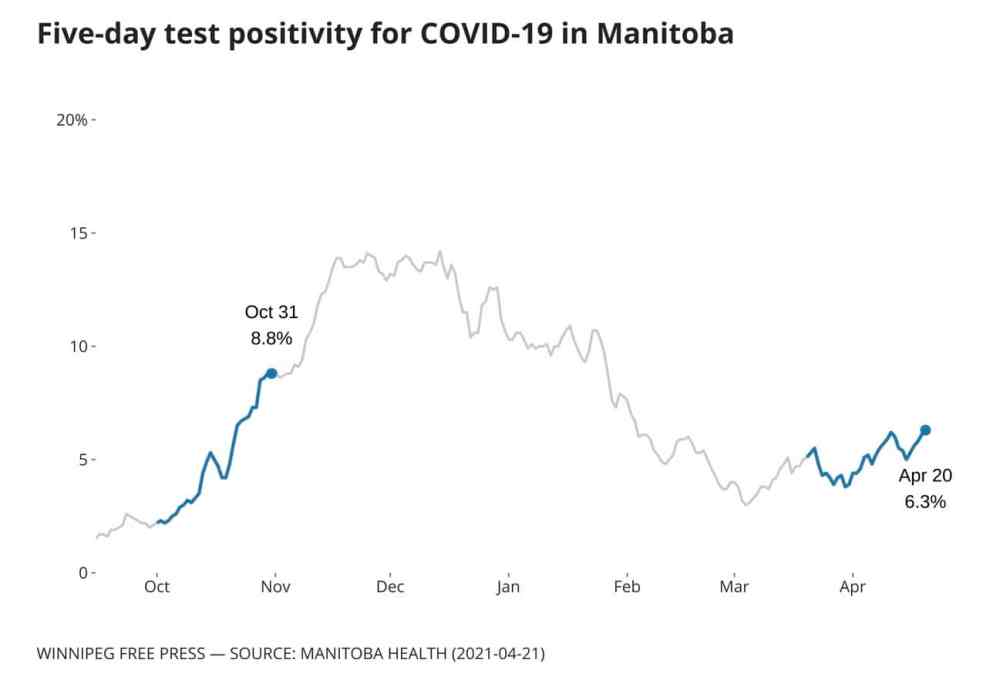
Case counts feed into restrictions
Heading into the third wave, most Manitobans were already living with much stricter public health rules than before the post-Thanksgiving spike in COVID-19 cases.
In October 2020, daily case counts averaged 120. Over the past month (March 20 to April 20), that number reached 103. New third-wave restrictions were added Tuesday and public health officials have warned the next step could be a complete lockdown.
Economically, it makes more sense in the long run to lock down once than to go back and forth imposing restrictions on businesses and individuals, says Jesse Hajer, assistant professor of economics and labour studies at the University of Manitoba.
The province’s unemployment rate wasn’t as high in March as it had been in the first wave of the pandemic, but there are still roughly 11,000 lost jobs that haven’t been recovered, and many of the emergency benefits and social supports brought in at the start of the pandemic haven’t been renewed.
Support for small businesses has improved in Manitoba, but low-wage workers, many of them women, are hardest hit. At this point, funding for schools, child care and community organizations is necessary, Hajer says.
Pandemic fatigue real but temporary
Even before the third wave hit, Canadians were already reporting their highest levels of depression and anxiety, according to an early February poll from Mental Health Research Canada. There was a 70 per cent increase between the first and second waves in respondents reporting they were highly depressed.

The resulting mental health crisis is an “echo pandemic,” says Winnipeg clinical psychologist Dr. Andrea Piotrowski.
The impact of isolation is taking its toll, but there are silver linings to look for in the third wave, she says. Thinking of this as a temporary experience, and being grateful for even little things — such as connecting with far-flung family members via virtual game nights, or learning to bake — can help. So can getting outside, being active and focusing on success stories from other countries that are further ahead in their pandemic response, she says.
“People are tired and they are fatigued, and we can almost see the light at the end of the pandemic tunnel, in terms of we are so close, but we really have to give just that extra push, that extra effort… In order for us to not go into a fourth wave, we do need to really think of, again, this is temporary,” Piotrowski says.
katie.may@freepress.mb.ca
Twitter: @thatkatiemay
michael.pereira@freepress.mb.ca
Twitter: @__m_pereira


Katie May is a multimedia producer for the Free Press.
Our newsroom depends on a growing audience of readers to power our journalism. If you are not a paid reader, please consider becoming a subscriber.
Our newsroom depends on its audience of readers to power our journalism. Thank you for your support.