Hep C
It's life-threatening, yet hardly understood
Advertisement
Read this article for free:
or
Already have an account? Log in here »
To continue reading, please subscribe:
Monthly Digital Subscription
$1 per week for 24 weeks*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Billed as $4.00 plus GST every four weeks. After 24 weeks, price increases to the regular rate of $19.95 plus GST every four weeks. Offer available to new and qualified returning subscribers only. Cancel any time.
Monthly Digital Subscription
$4.99/week*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Billed as $19.95 plus GST every four weeks. Cancel any time.
To continue reading, please subscribe:
Add Free Press access to your Brandon Sun subscription for only an additional
$1 for the first 4 weeks*
*Your next subscription payment will increase by $1.00 and you will be charged $16.99 plus GST for four weeks. After four weeks, your payment will increase to $23.99 plus GST every four weeks.
Read unlimited articles for free today:
or
Already have an account? Log in here »
Hey there, time traveller!
This article was published 17/07/2014 (4265 days ago), so information in it may no longer be current.
Robert Walker resented the probing questions from a doctor about his alleged alcohol consumption.

He was called into the physician’s office more than once following checkups when blood tests detected elevated liver enzyme levels.
“He was telling me to quit drinking,” Walker recalled recently.
Walker protested he was not a heavy drinker — he even got his wife to come in to vouch for his moderate alcohol-consumption habits.
The Walkers failed to convince the MD.
When that physician retired, Walker found a new doctor. But the troubling questions persisted.
“(The new doctor) said, ‘I need to ask you a hard question: How much do you drink?’ “
Walker was thinking ‘Oh no, not again.’
But after the second physician received assurances from Walker and his wife that Robert wasn’t a boozer, the doctor ordered a different blood test.
Four years ago, Robert Walker, now 62, discovered he had hepatitis C.
Hepatitis C, a liver disease spread by blood-to-blood contact, is little understood — even by many doctors.
Since screening began for the hepatitis C virus (HCV) in 1997, about 5,000 Manitobans have been identified with it.
But some experts believe there are many more people — anywhere from 5,000 to 15,000 more in the province — who are living with the potentially life-threatening disease without knowing it.
Most of them are likely baby boomers or those born shortly after the boom. So far, the vast majority of those diagnosed have fallen in those age groups.
A large number obtained the disease through recreational drug use in the 1960s and 1970s. Many contracted it through transfusions with tainted blood before proper screening procedures were put in place. Others likely got infected at tattoo parlours before those businesses started taking greater precautions. Some believe they got it while serving in the military decades ago, at a time when large-scale immunizations were carried out without the same precautions taken today.
Since the virus works slowly, often producing few if any symptoms for years, it can go undetected until the liver of an infected individual is severely damaged.

“We’re seeing more patients now presenting (for the) first time with advanced liver disease than I’ve ever seen, and I’ve been at this for 21 years,” said Dr. Kelly Kaita, director of the viral-hepatitis investigative unit at Health Sciences Centre and one of four liver specialists in the city.
Kaita — and the Canadian Liver Foundation — recommend family physicians order a simple, one-time blood test to anyone born between 1945 and 1965 to screen for the disease, especially for patients who shared needles while injecting drugs, snorted cocaine (the virus can be spread through microscopic amounts of blood, and the nasal passages of those who snort coke are prone to bleeding), received blood transfusions before 1990 or had body piercing and tattoos done.
Kaita said Winnipeg doctors who work with immigrant populations or with marginalized persons in the core area “do a fantastic job in testing” for HCV, and MDs in the suburbs should be just as vigilant. The test, which costs less than $10, is not usually conducted as part of blood work done during an annual checkup.
“I think the physicians in the suburbs, where their practice is made up of a different patient demographic, they probably aren’t testing. But guess what? They should be testing (if the patient is a baby boomer or in a high-risk group),” he said.

Dr. Michael Routledge, the province’s chief public health officer, said the hep C screening issue was raised earlier this month during a conference call involving public officers from coast to coast.
Increased screening is being discussed, in part, due to promising new treatments for hepatitis C, he said.
“This is a really actively evolving area,” Routledge said, adding any new recommendations would likely be made on a national level.
Currently, the direction to doctors is to test for hepatitis C if a patient is from an at-risk group. There is no direction from Manitoba public health to screen on the basis of the patient’s age, something that is now being discussed nationally.
“We certainly wouldn’t discourage testing, but we don’t have any specific recommendations around age groups,” Routledge said.
He believes the number of Manitobans who may unknowingly have hepatitis C is likely in the lower end of the range estimated by some experts — more like 5,000 or so more, as opposed to an additional 15,000.
Canadian estimates of how many people may have the disease range from 0.8 per cent of the population to 1.5 per cent, Routledge said. If, say, one per cent of Manitobans have the disease (those already diagnosed plus those yet to be diagnosed), that would add up to about 12,000.
The Canadian Liver Foundation sponsored a survey of general practitioners a little over a year ago that set off alarm bells about the lack of knowledge on hepatitis C. Only about one-third of the 300 GPs surveyed felt they knew a lot about the disease, and more than half did not know that it could even be cured.
“We were absolutely appalled by the lack of knowledge of family physicians, most notably that hep C is curable,” Kaita said.

Dr. Tamara Buchel, executive director of College of Family Physicians, said she would agree many GPs don’t know enough about the disease, particularly when it comes to emerging treatments.
But she said there is “a little bit more awareness” about hep C than there was a decade ago.
As for whether the disease can be cured, Buchel said many GPs may have genuinely questioned whether anyone is ever rid of the virus.
“I think if someone just came up the street to me and said, ‘Can hep C be cured?’ My instant answer is ‘no,’” said Buchel, who is also a practising physician.
“I am under the impression, as I think a lot of doctors are under the impression, that it still could, at some point in the future, reactivate. I’m not sure if every shred of virus goes away completely from the person’s body.”
But liver experts say it can disappear and does.
“If you were to ask a group of liver specialists who deal with hepatitis C whether or not hepatitis C is curable — in other words it’s gone for life, no chance of reactivation — 10 out of 10 of us would say absolutely yes,” said Kaita.
He said that doesn’t mean the patient won’t still face ongoing health issues brought on by the virus, and it doesn’t mean patients can’t reacquire the disease. But they can be cured.
In his unit at Health Sciences Centre, patients receive a blood test once a year for two years after a successful treatment. Over the past two decades, Kaita said he has not seen one relapse once this amount of time has elapsed.
Specialists are confident about a treatment outcome at the six-month mark, but test longer out of an abundance of caution, he said. “Our impression, based on fairly lengthy followup of these patients, is that you are truly cured of your disease.”

Every Thursday, in a small meeting room at the Manitoba office of the Canadian Liver Foundation in downtown Winnipeg, a group of past and current chronic hepatitis C patients gather for mutual support. Turnouts range from about six to 10 people.
Recently, when the Free Press paid a visit, the group shared stories about failed treatments and successful cures, bemoaned the lack of public and physician understanding of the disease and shared war stories about debilitating drug treatment side-effects.
Most agreed to be quoted by name and pose for photographs. Two of them have had liver transplants due to hepatitis C, while another is close to needing one.
A few believe they got the disease during mass immunizations while serving in the military, some believe they contracted it though blood transfusions and a few admit may have picked up the virus through recreational drug use in their younger days. Virtually all are baby boomers.
Several only learned of their illness after they were hospitalized, and all agreed more family doctors need to get up to speed on the disease.

“GPs haven’t got a clue,” said Brad Mastervick, a 61-year-old former soldier who is now undergoing his third attempt at treatment employing a cocktail of drugs that can produce side-effects ranging from extreme fatigue and depression to anxiety and anger.
“They used to line us up, give us our injections, all with the same gun,” Mastervick said of his military experience dating back to the 1970s, well before testing began for Hep C.
It wasn’t until late 1998 or 1999 that he discovered he had contracted the virus when a life insurance company turned him down for coverage. For years he had suffered regular bouts of fatigue and didn’t know why. Doctors suggested he had the flu or mononucleosis, he said.
Mastervick is currently participating in a gruelling 48-week treatment regime that includes a weekly injection of interferon and five tablets daily of ribavirin. While he’s on treatment, he also receives a weekly injection to keep his hemoglobin up and takes different pills to help him sleep, combat pain and stabilize his moods — or as Mastervick bluntly puts it, “so you’re not ripping people’s heads off.”

Bert Vledder, who spent 13 years in the military in the 1970s and 1980s, was diagnosed with hepatitis C while in hospital in 2005.
“I had just come back from a cruise, and I was really feeling terrible. I was in the hospital for about a week,” he said.
The disease, caught very late, has taken a tremendous toll on Vledder. He’s been through treatment four times and has yet to kick the disease. Twice he’s been in a coma.
In 2010, his liver had deteriorated to the point he underwent a liver transplant in Edmonton.
“When I got there the doctor told me that if they didn’t have an organ for me within a couple of days, that was it. Game over,” Vledder said.
A friend who visited him shortly before the transplant said he looked “like a corpse.”

Vledder has a new liver, but he still has hepatitis C. He’s hoping a promising new drug that was recently licensed but has yet to be covered by pharmacare in Manitoba will offer a cure.
Meanwhile, he has lost his job as a mechanic for an airline because his employer was worried that he might cut his skin and infect co-workers.
Another member of the support group, Heike DeGraff, has late-stage liver disease due to hep C. Like Vledder, she was also diagnosed while in hospital. The former Alberta women’s shelter director believes she contracted HCV 30 years ago when she had a blood transfusion when her youngest daughter was born. Now, 57, she fears she may soon require a liver transplant.
She’s started treatment twice over the years but was pulled off of it before it ran its full course. “I couldn’t handle it. I’m what they call a non-responder,” DeGraff said.
She is constantly fatigued and suffers from swollen joints, a product of her liver disease. She goes for an ultrasound every three months and has blood work done every couple of weeks. “It wreaks havoc on your system. It destroys all your organs and your joints and connective tissues,” DeGraff said of the disease.
While DeGraff is hoping promising new drugs that are starting to hit the market will offer her the hope of a cure, two other women in the support group have been able to rid themselves of the disease using conventional treatments.

Jacquie Maytwayashing, 48, learned she had HCV in 2006. She received a new liver in 2010.
“When I first found out I had hepatitis C, they told me that I carried the disease for 25 to 30 years,” she said.
She believes she contracted the virus when she had a blood transfusion as a teen after her appendix burst.
She was too ill to undergo treatment before receiving her new liver.
“It would have finished me off,” she said. “So they waited for me to have a liver transplant and then do treatment.”
She only had to undergo 24 weeks of treatment — half the time most patients must endure. Twelve weeks into the program, the virus was already gone, said Maytwayashing, who works as a teaching assistant with special-needs children.
Unlike many other patients, she also was mainly free of side-effects through treatment. “I just whizzed through it.”

Tina Lussier, a former marketing director for a local nightclub, finished her last interferon/ribavirin treatment last August. She went through the 48-week regime after lasting only six months in her first try. The initial treatment didn’t work.
“My hepatologist said I was the only patient he ever had to make it through the entire year the second time around and be cured,” she said.
Lussier, who is now self-employed, managed to work during her treatment — many patients can’t — because she could rest when she needed to. She credits her grown-up children for helping her to get through the depression caused by the treatment drugs. “I had a few episodes where I lost it,” she said.
Although she was initially diagnosed with hep C in hospital in 2002, she didn’t immediately undergo treatment. There is a lengthy list of conditions patients must agree to before entering treatment, including counselling, a psychiatric assessment (due to the side-effects of the drugs) and the agreement to abstain from alcohol.
“I didn’t want to quit drinking,” Lussier said with a laugh.
While it’s believed thousands of middle-aged Manitobans may unknowingly have hepatitis C, the good news is the number of new infections occurring these days is believed to be quite small.
“We’re very lucky that there are very few truly new cases. Otherwise we would never catch up to this epidemic,” said Health Science Centre’s Dr. Kelly Kaita.
But more public awareness about HCV is needed, especially so folks with advancing liver disease can be treated.

On July 28, to coincide with World Hepatitis Day in Canada, the local chapter of the liver foundation will stage a rally at the Manitoba Legislative Building to spread the word about the importance of getting tested and to press the province to cover a pair of newly licensed drugs that have shown to be more effective while producing little or no side-effects.
Meanwhile, Walker, the man who had to convince his doctor he wasn’t a heavy drinker, underwent treatment last year without success.
“I got pulled (off drug therapy six months into a 48-week regime) last September as a non-responder,” he said recently.
Walker’s disease is at Stage 2-3 (Stage 4 being the most serious). He’s now pinning his hopes on a new generation of hep C drugs that could potentially be covered by Manitoba pharmacare by sometime next year.
larry.kusch@freepress.mb.ca
Hope on horizon, but comes with huge price tag
Hepatitis C patients are looking forward to the day they can receive provincial coverage for a new generation of drugs that offers much higher cure rates with little or no side-effects.
In recent months, Health Canada has licensed two new anti-viral drugs — Sovaldi, manufactured by Gilead Canada, and Galexos, a product of Janssen Inc., a division of Johnson and Johnson.
Not only do the new drugs offer improved cure rates, the treatment time is about one-quarter the length of current regimes.
But while they have been licensed in Canada, they are too costly for all but a few wealthy patients to afford since they’ve yet to be covered by provincial drug programs, including Manitoba’s pharmacare.
Sovaldi, for instance, retails for $647 per tablet in Canada. At one tablet per day over the course of a 12-week treatment, that adds up to close to $55,000.
Bianca Pengelly, Manitoba regional co-ordinator for the Canadian Liver Foundation, said she is aware of one wealthy individual who paid for Sovaldi out of her own pocket.
“She has only had the (12-week) treatment one time and she’s cured,” Pengelly said.
But the vast majority of patients will have to await the outcome of a national review process that will determine whether the new drugs should be added to provincial formularies.
The provinces will band together to negotiate a price with the manufacturers, a process that is expected to bring costs down. Then the Manitoba government will have to decide whether to cover them under pharmacare.
According to one estimate, pharmacare coverage is unlikely to be available for either new drug until sometime next year. When contacted by the Free Press recently, a provincial spokeswoman said the government could not offer a timeline.
Drug companies sometimes make their products available on a compassionate basis, but sources say patients need to be near death to qualify.
Until a couple of years ago, the success rate of drug treatment for hepatitis C was in the 45 to 50 per cent range. Over the last two years, that’s been improved to 60 to 65 per cent.
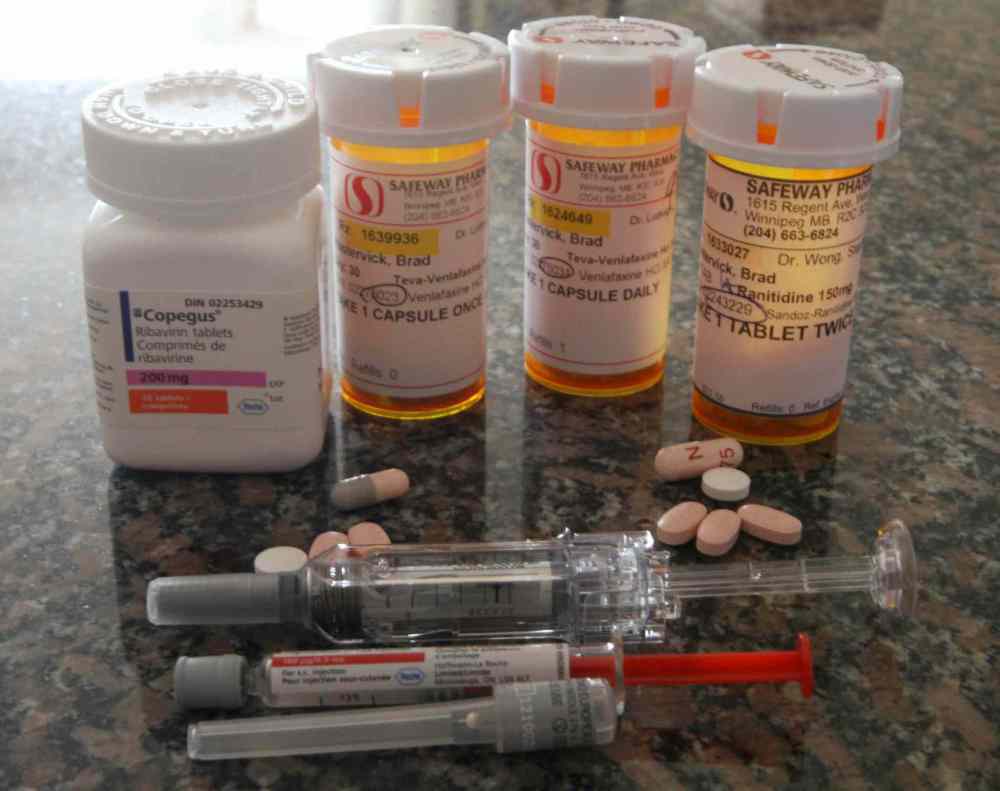
The new drugs, as currently licensed, boost that effectiveness rate to 80 per cent or more. Soon, they will be bundled with different drugs that will increase their effectiveness to 95 per cent or more.
There’s also research that suggests if the two new drugs are used in combination the chances of a cure exceed 90 per cent, even for patients who have been unresponsive to conventional drug treatments.
Dr. Kelly Kaita, director of the viral hepatitis investigative unit at Health Sciences Centre, said he believes the new drugs will be approved, despite their high cost.
“I can’t see them (the provinces) balking at a product that brings cure rates so high and that is used worldwide,” said he said.
Kaita noted the drugs that are currently used are also very expensive, without being as effective.
For patients whose disease has not progressed too far, the new drugs are likely worth the wait, he said.
But it’s an especially frustrating waiting game for those with advanced hepatitis C virus (HCV). Many of these patients have already undergone multiple treatments without success.
And the side-effects from the current drug cocktail, which includes interferon, are described as horrible and “worse than cancer treatments.”
“It just about kills you,” said Winnipegger Bert Vledder, who has undergone four failed treatments and a liver transplant.
“It feels like the top of (your) head is coming off,” said Brad Mastervick, who is now partway through his third course of treatment.
“It felt like my skin was on fire,” said Tina Lussier, who successfully completed treatment last year.
Besides pain, the interferon’s side-effects range from extreme fatigue and a loss of balance to rage and suicidal depression.
Said Kaita: “Whenever we can drop interferon, it’s going to be a good day for patients.”
But that won’t happen yet. In their effort to rush Sovaldi and Galexos to market, the manufacturers consented to labelling requiring they be used with interferon and ribavirin. Treatment time, however, has been reduced to 12 weeks.
“The next generation of drugs that will probably come out end of 2015, beginning of 2016, will be interferon-free,” said Kaita. “And that’s when the cure rates will start hitting high 90s.”
larry.kusch@freepress.mb.ca

