City clinic battles criticism of pay-for-plasma services
Critics question ethics, practicality of paid plasma donations
Advertisement
Read this article for free:
or
Already have an account? Log in here »
To continue reading, please subscribe:
Monthly Digital Subscription
$1 per week for 24 weeks*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Billed as $4.00 plus GST every four weeks. After 24 weeks, price increases to the regular rate of $19.95 plus GST every four weeks. Offer available to new and qualified returning subscribers only. Cancel any time.
Monthly Digital Subscription
$4.99/week*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Billed as $19.95 plus GST every four weeks. Cancel any time.
To continue reading, please subscribe:
Add Free Press access to your Brandon Sun subscription for only an additional
$1 for the first 4 weeks*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Your next Brandon Sun subscription payment will increase by $1.00 and you will be charged $17.95 plus GST for four weeks. After four weeks, your payment will increase to $24.95 plus GST every four weeks.
Read unlimited articles for free today:
or
Already have an account? Log in here »
Hey there, time traveller!
This article was published 08/08/2017 (3199 days ago), so information in it may no longer be current.
It’s a relatively nondescript ad tucked under the part-time job tab on Kijiji, a red banner declaring it urgent: “Do something amazing today… donate plasma, save a life, get paid!”
It takes about 90 minutes to donate, Prometic Plasma Resources advises prospective donors, but there’s a $100 bonus if a person donates eight times this month. That bonus is on top of the $25 for each donation.
“We’re not trying to compete with Canadian Blood Services (CBS),” said Bill Bees, the company’s vice-president of plasma technologies. “We’re trying to complement what they’re doing.”
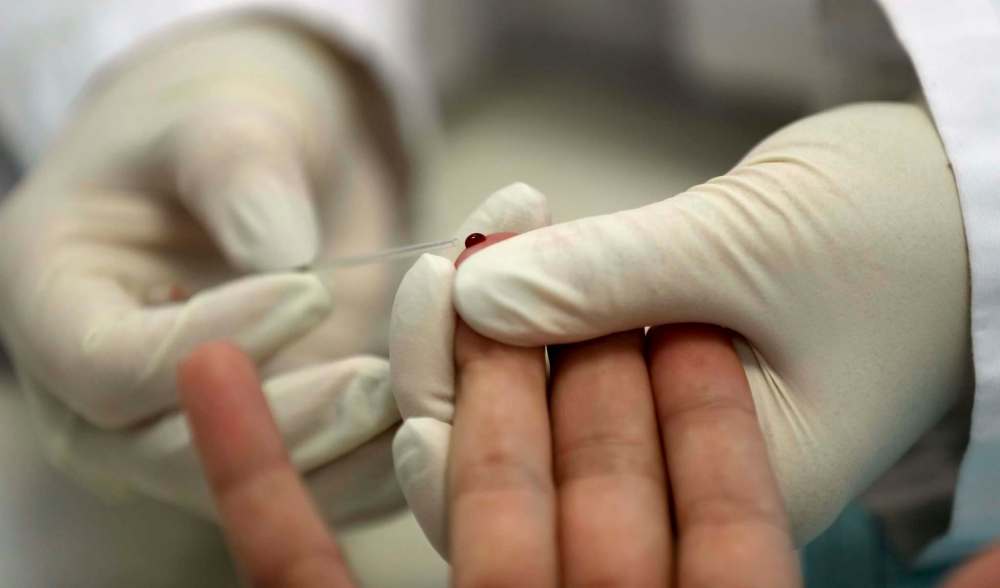
Paying for plasma is a contentious issue in Canada, increasingly so in recent years after private pharmaceutical manufacturer Canadian Plasma Resources (CPR) opened a paid plasma centre, first in Saskatoon and then in Moncton, N.B. That meant Canada has three plasma clinics that pay donors.
The controversy flared up recently after BloodWatch, a non-profit that advocates for a voluntary, public-only blood donation system, released a letter obtained through access-to-information that shows CBS had warned Health Canada against the proliferation of pay-for-plasma facilities. Health Canada licensed the Moncton facility anyway.
Like always, Prometic warrants a media mention, usually as the long-standing original pay-for-plasma clinic in Winnipeg. But, Bees said, that description doesn’t capture what Prometic does.
“It was a feel-good thing,” he said of its origin, which dates back to the early 1970s. The facility was bought in 2015 by U.S.-based Prometic.
At the time, Winnipeg’s Dr. John Bowman was researching Rh disease, which is when a pregnant woman’s immune system sees a fetus’s red blood cells as foreign and her antibodies begin to attack them. It hurts the fetus and increases the risk of a stillbirth.
Bowman’s work led to the creation of Rho(D) immune-globulin, or WinRho, a medication that prevents the woman’s body from forming the antibodies. The ‘Win’ is a nod to Winnipeg.
Today, collecting plasma and developing it into intravenous immunoglobulin, which can be used to treat a number of rare disorders, comprises the bulk of Prometic’s Canadian operations.
The collection centre paid its donors then — as it does now — because, Bees said, “We feel ethically, it’s a good thing to do.”
That isn’t the norm in Canada.
After the HIV epidemic in the 1970s and ’80s, a national inquiry looking into the safety of Canada’s blood system recommended against paying for donations. The Winnipeg lab has been an exception because of its focus on rare disorders.
It has grown, Bees said, from six beds when it first opened on Kennedy Street to 18 beds on the Smart Park campus at the University of Manitoba, where it has been since 2010.
The facility is on track for 300 donations per week, he said. A clinical trial is underway in the United States for a new drug to treat excessive blood-clotting. Prometic plans to try to license that drug in Canada first.
Kat Lanteigne, executive director of BloodWatch, said it’s important to understand not just the difference between the specialty work Prometic does and new clinics, but the real concern BloodWatch has with new pay-for-plasma clinics.
“Often, the argument gets reduced to the moral argument of whether you should pay people to sell their body parts or not,” Lanteigne said, but “when they say paying for plasma, it means that a private corporation is paying people to sell their plasma so they can export it from Canada and sell it on the international market.”
Plasma has to be processed via fractionation, which the CPR can’t do in Canada, so it ships plasma overseas. (Prometic has a fractionation plant right next door). CBS has said it is not under any obligation to purchase from CPR.
While Bees and Lanteigne disagree about whether paying for donors negatively affects voluntary donations, Lanteigne said she’s mostly concerned about safety.
If there is a blood-borne virus, CBS can trace it back through donor records across the country, she said, whereas “if there’s a private corporate model, we have no access to those donor records.”
Ultimately, Lanteigne said, CBS needs to start collecting more plasma.
“There are private companies who are vying to say, ‘We really want to help,’” she said of the shortage, but “we just need CBS to do their job.”
CBS declined to comment and directed the Free Press to a statement posted to its website in January.
The organization has an “ambitious” plan to beef up its plasma sufficiency so it can eventually supply half of the immunoglobulin Canadians need from voluntary and unpaid Canadian donors. By 2024, CBS is hoping to have up to 40 plasma collection sites across the country, a plan that requires more than 144,000 new donors each year.
Even with that plan, Bees said CBS will still need to look elsewhere for the other half of its immunoglobulin supply.
That’s where he hopes Prometic can step in.
jane.gerster@freepress.mb.caTwitter: @Jane_Gerster
History
Updated on Tuesday, August 8, 2017 7:03 AM CDT: Photo added.


