Sensitive soul
Deeply caring woman failed by medical system that didn't care back
Advertisement
Read this article for free:
or
Already have an account? Log in here »
To continue reading, please subscribe:
Digital Subscription
One year of digital access for only $1.44 a week*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Billed as $5.77 plus GST every four weeks. After 52 weeks, price increases to the regular rate of $19.95 plus GST every four weeks. Offer available to new and qualified returning subscribers only. Cancel any time.
To continue reading, please subscribe:
Add Free Press access to your Brandon Sun subscription for only an additional
$1 for the first 4 weeks*
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*Your next Brandon Sun subscription payment will increase by $1.00 and you will be charged $17.95 plus GST for four weeks. After four weeks, your payment will increase to $24.95 plus GST every four weeks.
Read unlimited articles for free today:
or
Already have an account? Log in here »
Hey there, time traveller!
This article was published 04/12/2021 (1636 days ago), so information in it may no longer be current.
Floating along Nutimik Lake on one of her last trips to the beach, Jennifer Evers talked about dying.
Her drainage tube was concealed under her swimsuit, stuck in place with waterproof bandages, as she reclined on an inflatable chair under a sunny sky, legs dangling in the water, soaking in the Whiteshell during that final summer.
The 46-year-old knew she was dying — had known long before doctors believed her.

She was vindicated, then devastated, when she finally got the diagnosis alone in a protocol-heavy hospital room four months into the pandemic. Stage 4 incurable stomach cancer. She told her family she was right. She told them it shouldn’t have been this way.
But that day on the lake last June, her sister Allison floating beside her, Jenn wasn’t worried about what little time she had left.
“She said she knew she was dying, but it was OK, because she was going to be part of nature,” Allison Evers says.
The memory is a joyful one; a placid moment near the end of what was, frankly, a hard life.
Three months later, as her mother kissed her goodnight, Jenn took her last breath, her cause of death a post-chemotherapy infection. She died 14 months after the cancer diagnosis, and more than 25 years after she was diagnosed with obsessive-compulsive disorder, extreme anxiety and depression. Those earlier diagnoses fatally delayed the last one, her family believes, and they don’t want it to happen to anyone else.
“It should never have happened, that’s what we can’t live with. And we feel terrible about it because we knew she was sick, but yet the doctors were not taking her seriously, were not finding anything, were saying, ‘No, Jenn, there’s nothing wrong,’ but here our beautiful sister is suffering and dying,” her oldest sister Lisa Evers says.
She carries guilt for trusting the medical system over her sister before it was too late. No one in the family suspected cancer — they’d already seen Jenn through years of what Lisa called “a survival game” of managing her OCD, anxiety and depression.
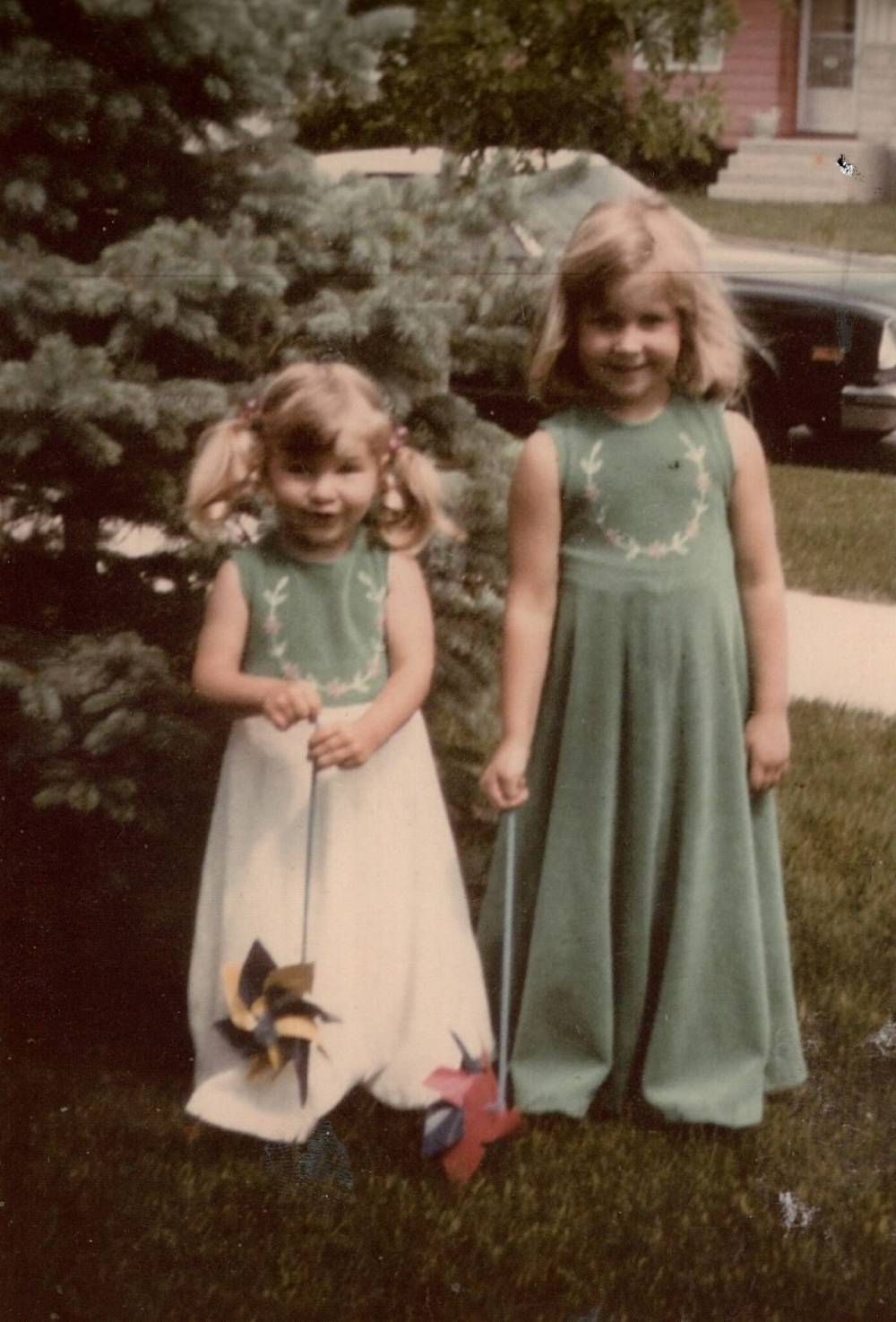
Jenn was born in Selkirk, the youngest of the three girls. Her mother, Tannis Evers, recognized some of her own family history in her sensitive and perceptive little girl. Symptoms of OCD started showing up when Jenn was around nine years old. She wouldn’t be formally diagnosed until she was a young adult.
“I always knew, from the time she was little, even really little, there was just something there. I could sense that… life was going to be hard for her,” Tannis says.
Jenn was easily overwhelmed and her temper percolated. Her teachers often didn’t understand how to communicate with her. Her family realized she was internalizing other people’s moods and taking everything personally.
“But on the flip side, she would know if a person was not being truthful about how they were feeling,” Tannis says.
“One of the counsellors that she had once told her that she had a deep way of knowing,” Allison adds.
Jenn told her family she was dying four or five years before she did. During those years, her symptoms progressed from acid reflux to trouble swallowing to foamy regurgitations and excruciating stomach pain that sent her to the ER several times.

On one of those visits, about two months before the cancer was diagnosed, a doctor suggested Jenn was simply constipated.
A family member often accompanied Jenn to appointments, and Lisa made notes. She wrote down doctors’ exasperated comments. “What do you want me to do for you?”
The dismissive ones. “You’re too young to be sick all the time. Maybe you need a pet.”
The ones uttered in condescending tones. “I’ve sent you to several specialists and none of them have found anything wrong with you. Why do you think that is, Jenn?”
The list of pills Jenn was taking for her mental illnesses or her predisposition to do her own research may have prejudiced those doctors’ perceptions of Jenn, her family says. For whatever reason, doctors weren’t listening.
“We believe that it was because of her mental-health history,” Lisa says.

By the time an attentive ER doctor ordered more tests in July 2020, the cancer had spread beyond Jenn’s stomach walls. When it came time to stop treatment, another doctor gently took the family aside.
“She said, ‘I just want you to know that Jenn has been failed by the system,’” Lisa recalls.
So many of the what-ifs the Evers family is left with can only be answered now in the form of systemic change. They’re calling for better mental-health education for medical professionals, improved public funding of mental-health services, affordable housing, and basic kindness. All of it would’ve improved Jenn’s quality of life and, they believe, could help so many other Manitobans, especially those who don’t have such a strong network of family support.
Before her deteriorating mental health forced her to stop working at 40 and go on disability, Jenn cared for others as a health-care aide at Betel personal-care home in Selkirk, and later as a home-care worker. Residents and clients loved her, her family says.
“I think because she was so sensitive and could get hurt so easily, she in turn wanted other people to feel good and didn’t want them to be hurt,” Lisa says.
The strain of trying to manage more clients in less time got to be too much. Because her disability payments didn’t cover rent, she was a grown woman living with her parents, watching those around her hit milestones she felt she couldn’t reach. Even with support from her family, Jenn became bitter.
‘She was so frustrated because she couldn’t reach her full potential. She wanted to be independent, to have her own apartment, to be able to do home care or a job that (meant) she could display her talents and use her kindness and compassion,” Lisa says.

Gravitating to the outdoors, Jenn preferred a quiet life in the country. She was more than content to sit with coffee on the deck, spotting deer. In the winter, she pitied the wild animals, loading her car with food to bring back and keep them sated through the cold.
It wasn’t a kindness she reserved for four-legged creatures — Jenn was known to take her home-care clients grocery shopping or drive them to church on her own time. She hauled a bed-bug-infested mattress out of a friend’s apartment and sanitized the place, taking on other people’s problems even though she was still grappling with her own.
She wanted to see more empathy in the world, and wasn’t afraid to confront anyone who was being unfair. She’d say aloud the gutsy things other people didn’t think they could.
“Generally when she did call things as they were, it was to try and improve things,” Allison says.
“For sure,” Lisa agrees. “It was because a change was necessary.”
That’s what her family is trying to do now.

With a little more publicly funded support and a bridge between the medical and mental-health systems, they say, she could have had the life she wanted — as could so many other Manitobans who struggle with mental illness.
As Lisa says, “We just want to help people that are going through the same thing that our sister went through.”
katie.may@winnipegfreepress.com

Katie May is a multimedia producer for the Free Press.
Our newsroom depends on a growing audience of readers to power our journalism. If you are not a paid reader, please consider becoming a subscriber.
Our newsroom depends on its audience of readers to power our journalism. Thank you for your support.
History
Updated on Thursday, December 16, 2021 11:01 AM CST: Adds photo cutlines

